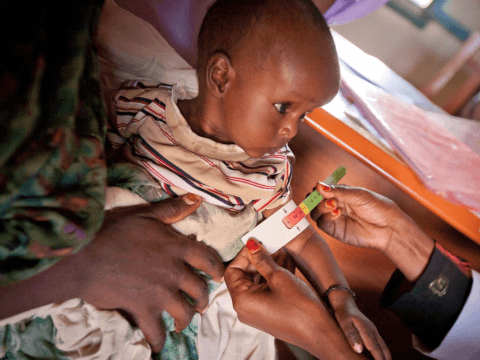
Community-based Management of Acute Malnutrition
Addressing Wasting
Between 2010 and 2024, 88% of the 875,245 severely wasted children we treated made a full recovery.
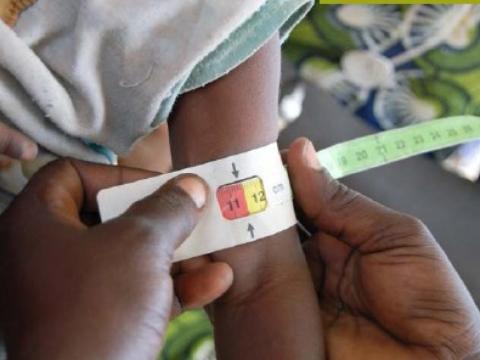
Acute malnutrition, also known as ‘wasting’, increases the risk of serious illness or death. Globally, an estimated 45 million children under five years suffer from wasting, yet only 1 in 3 children receive the necessary treatment. Wasting occurs as a result of recent rapid weight loss or a failure to gain weight, often due to insufficient food intake or illness. Severe wasting is responsible for 1 in 5 deaths among children under 5, causing the loss of more than 1 million young lives each year, either directly through severe malnutrition or indirectly by weakening the immune system and increasing deaths in children suffering from common illnesses such as diarrhoea and pneumonia. Children with severe wasting are nearly 12 times more likely to die than well-nourished children. This issue is not limited to humanitarian crises, but is also prevalent in situations of chronic food insecurity and limited access to healthcare - 75% of wasted children do not live in humanitarian contexts. The world is off-track to meet global wasting targets, with 43% of countries showing insufficient progress, no improvement or worsening trends.
Since 2005, World Vision’s programmes have focused on the prevention and treatment of wasting, both in fragile and stable contexts in 35 countries, almost half of which are in the top 20 fragile states (Fragile States Index 2024). World Vision was an early adopter of the Community-based Management of Acute Malnutrition (CMAM) model, which empowers communities to both identify and treat malnourished children.

In 2024, 180,774 children under five years of age were treated for wasting in CMAM programmes across 15 countries, achieving a cure rate of over 86% and preventing the vast majority of these children from dying. (Data from 15 of the 20 countries implementing CMAM).
In addition, 40,627 pregnant and breastfeeding women in 7 countries received targeted supplementary feeding support to prevent and address malnutrition during critical periods.
Since 2010, World Vision’s CMAM programmes have treated more than 3.18 million women and children under five in 35 countries. Based on lives saved analysis, we estimate that 103,958 children’s lives were saved between 2010 and 2021 as a result of these efforts.
World Vision plays an active role in technical and advocacy platforms on CMAM and wasting. We are engaged in global research projects on wasting, and contribute data from our global CMAM database to research initiatives and engage in policy-shaping dialogues. Notably, World Vision’s CEO, Andrew Morley, represented the organisation on the UNICEF-led Action Review Panel on Child Wasting. We also advocate for global action through collaborations such as the Global Action Plan on Wasting, and the Wasting Reset initiative. At the 2024 Paris Nutrition for Growth Summit, our commitments focused on advocacy and policy change for the prevention, early detection, and treatment of child wasting as well as treatment of wasting in children and supplementary feeding for pregnant and breastfeeding women through CMAM programmes.
World Vision is also a member of the UNICEF/WHO Technical Advisory Group on Wasting and Nutritional Oedema (Acute Malnutrition), contributing expertise to shape global standards and approaches.